The Tuskegee Syphilis Study stands as one of the darkest medical experiments in U.S. history. Conducted between 1932 and 1972, it was a government-run study that intentionally withheld treatment from hundreds of Black men infected with syphilis – all without their informed consent. For four decades, these men were misled, denied care, and exploited under the guise of public health research.
This shockingly unethical experiment did more than just harm its direct victims – it deeply eroded trust in the medical system, particularly within Black communities. The repercussions of Tuskegee are still felt today, influencing medical ethics, public health policy, and surely contributing – understandably – to the vaccine hesitancy we see today.
In this article, we’ll break down what happened, why it mattered, and what lessons we can learn to ensure such a tragedy never happens again.
Recommended by The Clean Living Path
Protect Your Family from EMF
Aires Tech uses peer-reviewed, scientifically validated technology to harmonize EMF signals from phones, routers, and smart devices. Trusted by doctors, athletes, and parents worldwide.
Get 25% Off Aires Tech →Discount auto-applies at checkout — no code needed. Free shipping over $99.
What Was the Tuskegee Syphilis Study?
In 1932, the U.S. Public Health Service (PHS), working with the Tuskegee Institute, launched a study to observe the natural progression of untreated syphilis in Black men. The study took place in Macon County, Alabama, one of the poorest regions in the country.
The Participants: Misled and Exploited
- 600 African American men
 were enrolled in the study.
were enrolled in the study. - 399 had syphilis, while 201 served as a control group (not infected).
- The men were told they were being treated for “bad blood,” a vague local term used for various health issues.
- They never received proper treatment – even after penicillin was discovered as a cure in the 1940s.
The government’s justification? They wanted to study how syphilis affected the body over time. Instead of providing the cure, researchers deliberately withheld treatment, allowing the men to suffer, deteriorate, and even die – all for the sake of science.
The Racial and Ethical Violations
Why Target Black Men?
The Tuskegee Study was essentially built on pretty racist medical beliefs. During this era, many researchers falsely believed that Black people had biologically different bodies and that their sexual behavior was more promiscuous and reckless, making them more susceptible to sexually transmitted diseases.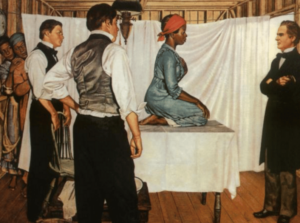
Rather than providing real healthcare, the study treated these men as test subjects, not human beings. This reflects a larger history of medical racism in the U.S., including:
- Henrietta Lacks (1951): A Black woman whose cancer cells (HeLa cells) were taken without her knowledge and used for research.
- Forced Sterilizations (1900s-1970s): Thousands of Black, Native American, and Latina women were sterilized under government-backed eugenics programs.
- Experiments on Enslaved Women (1800s): Dr. James Marion Sims, known as the “father of gynecology,” experimented on enslaved Black women without anesthesia.
The Deception and Lack of Consent
- Participants were never told they had syphilis.
- They were offered free meals, medical exams, and burial insurance as incentives.
- When the study began, there was no effective cure, but once penicillin was discovered in 1943, the government still refused to treat them.
Even after World War II, when the Nuremberg Code established ethical guidelines for human experiments, the U.S. government ignored these principles and continued the study for another 25 years.
The Exposure and Fallout
In 1972, a whistleblower, Peter Buxton, leaked details of the study to the press. Journalist Jean Heller of the Associated Press broke the story, sparking national outrage.
The Immediate Consequences
- The study was shut down within months.
- A class-action lawsuit was filed, leading to a $10 million settlement for survivors and their families.
- The U.S. government established new medical ethics laws, requiring informed consent and oversight for human experiments.
- In 1997, President Bill Clinton issued a formal apology, stating:
“What was done cannot be undone. But we can end the silence, we can stop turning our heads, we can look at you in the eye and finally say, on behalf of the American people, what the United States government did was shameful.”

The Lasting Impact on Public Health
The Tuskegee Experiment seriously damaged trust between Black Americans and the medical system. This distrust manifests in various ways:
- Lower participation in clinical trials – Black individuals are underrepresented in medical research due to historical mistreatment.
- Vaccine hesitancy – The skepticism surrounding COVID-19 vaccines was heavily influenced by memories of Tuskegee.
- Avoidance of healthcare – Many Black Americans avoid routine medical care due to fear of mistreatment.
This skepticism is not irrational as it’s often assumed to be – it’s rooted in real historical betrayals like Tuskegee.
Medical Reforms After Tuskegee
After the experiment was exposed, the U.S. government made significant changes to protect human subjects in medical research:
- 1974 National Research Act: Required Institutional Review Boards (IRBs)
 to oversee experiments.
to oversee experiments. - Informed Consent Laws: Patients must now be fully informed about medical procedures and sign consent forms.
- Bioethics Commissions: Organizations were created to review ethical concerns in medical studies.
While these reforms were crucial, distrust in medicine remains – and public health leaders must actively work to rebuild credibility.
Lessons for Today’s Public Health System
To prevent another Tuskegee-like disaster, the medical system must:
- Prioritize Transparency: Be honest about medical risks and historical injustices.
- Increase Representation: More Black doctors, researchers, and public health leaders can help rebuild trust.
- Engage With Communities: Public health officials must actively listen to concerns and include marginalized communities in medical decision-making.
The Connection to Environmental Health
Medical racism doesn’t just affect healthcare – it also impacts environmental health. Communities of color are often:
- Exposed to more pollution (Flint water crisis, high lead exposure).
- Denied healthcare resources (fewer hospitals and clinics in Black neighborhoods).
- Less likely to be believed by doctors when reporting symptoms.
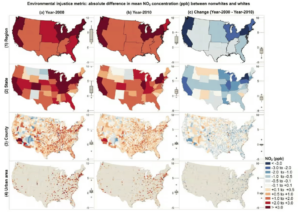
Understanding the legacy of Tuskegee is critical for addressing both medical and environmental injustices today.
Final Thoughts
The Tuskegee Syphilis Experiment is more than a tragic blemish in the history of the United States government – it is a stark reminder of the consequences of unchecked medical authority, racial discrimination, and unethical research practices. For four decades, hundreds of Black men were deceived, denied treatment, and used as unwitting test subjects, all under the guise of scientific study. The ripple effects of this betrayal did not end when the study was exposed in 1972. Instead, it permanently altered the relationship between Black communities and the American healthcare system, fostering a deep mistrust that continues today.
A Lasting Legacy of Distrust
The lingering skepticism toward medical institutions is not baseless paranoia to be disregarded – it is rooted in a legitimate and long history of systemic neglect, racial bias, and exploitative research. Even with the establishment of informed consent laws, research oversight, and bioethics regulations in the aftermath of Tuskegee, distrust remains a significant barrier to healthcare access and public health initiatives. Issues like lower vaccination rates, reluctance to participate in clinical trials, and avoidance of preventive care are often traced back to the betrayal of Tuskegee and other instances of medical racism.
However, simply acknowledging this history is not enough. The challenge now is ensuring that past mistakes do not define the future of medicine and public health. Addressing the damage requires more than just legal safeguards – it demands a cultural shift in how healthcare institutions engage with historically marginalized communities.
Moving Forward: What Must Be Done?
Rebuilding Trust Through Transparency
Medical institutions must proactively communicate openly and honestly about public health policies, treatment risks, and research objectives. Secrecy and misinformation were the cornerstones of the Tuskegee deception – truth must be the foundation of modern healthcare reform.
Community-Led Public Health Initiatives
Addressing generational mistrust requires engagement at the community level. Healthcare professionals and researchers must work alongside local leaders, churches, and grassroots organizations to bridge the gap between medical science and public understanding.
Equitable Access to Quality Healthcare
The unethical treatment of Tuskegee participants was exacerbated by their limited healthcare options. Ensuring that all communities – regardless of race or socioeconomic status – have access to affordable, high-quality medical care is essential in preventing similar injustices.
Stronger Ethical Oversight in Medical Research
While Institutional Review Boards (IRBs) and ethical review processes were implemented after Tuskegee, modern research still faces ethical dilemmas, especially in underserved populations. Ensuring that no group is disproportionately burdened in clinical studies is crucial in preventing exploitation.
Why This Still Matters Today
The Tuskegee Experiment is not an isolated incident in history – it is part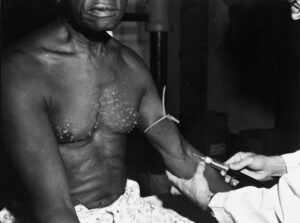 of an ongoing conversation about ethics, race, and medical integrity. Its lessons extend far beyond its victims, shaping how society approaches public health, research ethics, and healthcare accessibility. It is a constant warning of what happens when human lives are devalued in the name of science.
of an ongoing conversation about ethics, race, and medical integrity. Its lessons extend far beyond its victims, shaping how society approaches public health, research ethics, and healthcare accessibility. It is a constant warning of what happens when human lives are devalued in the name of science.
At its core, medicine should be about healing, never harm. The true measure of progress is not just in the advancements of technology and treatment but in the ability to recognize past failures, take accountability, and build a future where trust is no longer a privilege but a standard.
If the medical field is to regain full credibility, it must earn back what was lost – not through apologies alone, but through action, accountability, and an unwavering commitment to ethical care for all.



